Fungal Acne: A Dermatologist’s Guide to This Skin Condition
Learn about the causes of fungal acne, how it differs from regular acne, and the best treatments for this condition.
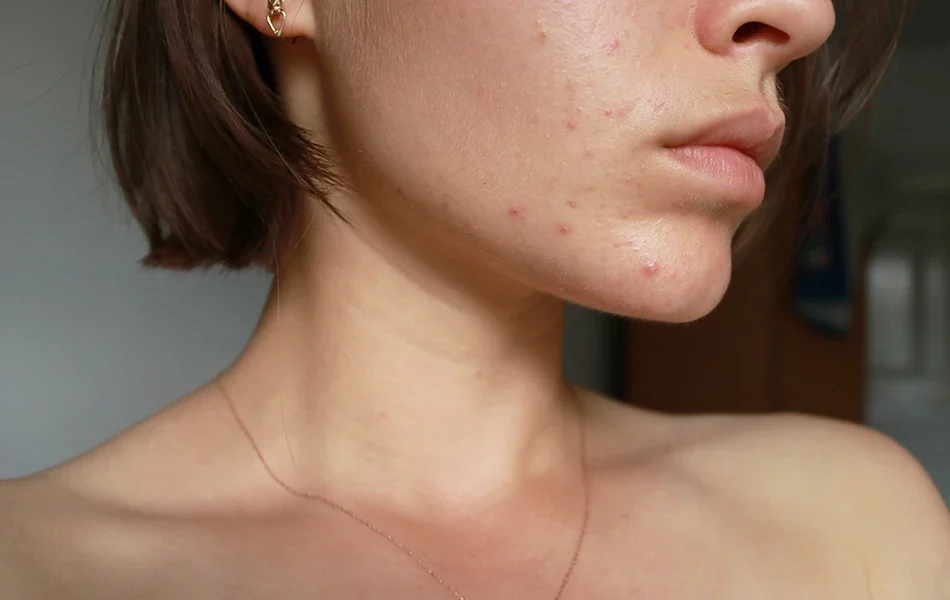
Do you have small red bumps on your skin that won’t go away?
Fungal acne is a frustrating skin condition that can make your skin feel sore, textured, sensitive, and itchy. The constant urge to scratch the itchiness may interfere with your daily routine, so learning about these pimples is essential for replenishing your skin.
Discover what fungal acne is, the common symptoms, and ways you can treat these pimples to achieve healthy skin.
Fungal Acne: What Is It?
Fungal acne, also known as malassezia folliculitis or pityrosporum folliculitis, is a common skin condition that derives from yeast overgrowth. Your skin’s hair follicles get infected by the fungus called malassezia yeast. You may need antibiotics or a cream-based antifungal treatment to revive your skin.
With a fungal overgrowth, you may experience red bumps or papules on your skin that are sore and itchy. If left untreated, those bumps can turn into whiteheads that contain yellow pus. This could also lead to more infections that cause swelling and inflammation.
Malassezia yeast is a lipophilic organism that feeds on your skin’s sebum. Everyone has this type of yeast on their skin, but it only becomes harmful when it enters damaged pores. Tight clothes, friction, and hair waxing are some instances that may trigger fungal acne breakouts due to skin damage.
Causes of Fungal Acne
Fungal acne can be caused by external factors like touching your skin frequently and using a hot tub or internal factors such as a compromised immune system and medication. Learning about the common reasons for fungal folliculitis can help you avoid these stubborn breakouts.
Below are some potential triggers for a fungal skin condition:
- Too much friction: Skin rubbing against skin can damage pores and increase the risk of yeast multiplying. You may experience chafing from exercise, hot weather, or irritating fabric from your clothes.
- Hair removal: Shaving, waxing, and plucking your hair could trigger inflammation in your skin’s hair follicles, which fosters the development of fungal colonization. Therefore, using a fresh razor every week is essential for healthy skin. You should also choose sugar wax instead of hard wax because it doesn’t cause inflammation.
- Touching your skin with dirty hands: An obvious trigger is the constant touching of your face. Everyone has germs on their hands, so transferring germs onto your skin will promote fungal infection.
- Using a hot tub frequently: Sitting in a poorly maintained hot tub can encourage yeast to develop in warm moisture. Cleaning your hot tub regularly and jumping in the shower afterward should prevent fungal infections on your skin.
- Wearing tight or sweaty clothes: Leaving damp clothes on gives malassezia yeast a chance to thrive in those moist conditions. Changing out of sweaty exercise gear or wearing loose clothes more often can protect your skin from fungal acne.
- Medication: Some antibiotics could reduce the good bacteria that regulate your skin. In turn, your skin is more exposed to germs and yeast that trigger itchy follicular eruptions.
How to Tell if You Have Fungal Acne? Symptoms and Identification
You might be wondering – how is fungal acne diagnosed? Fungal acne produces a range of physical symptoms related to swelling and redness. Most people experience severe itchiness or burning on the skin, as this fungus causes a skin rash.
Common symptoms of fungal acne include:
- Small, red bumps
- Inflamed hair follicles on your skin
- Very itchy and dry skin
- Spots usually appear on the face, chest, arms, and back
- Pus-filled bumps that look like whiteheads
- Swelling and redness
- Stinging sensation
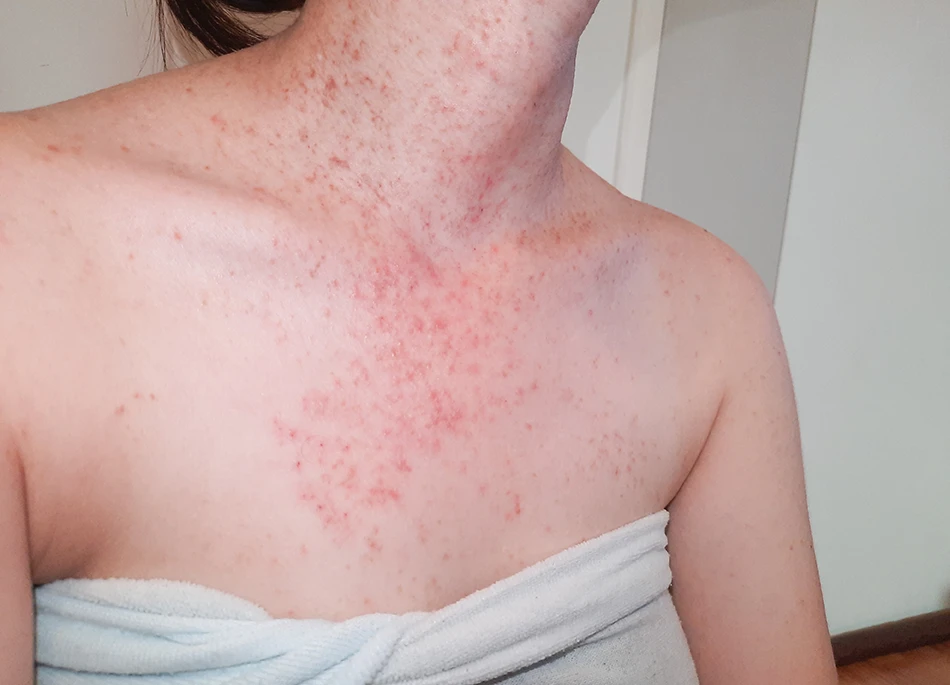
What does fungal acne look like?
Fungal acne looks like clusters of small, red bumps on your skin. These bumps usually cause swelling and redness in one area. In some cases, these bumps grow into painful whiteheads with a white-colored fluid inside them.
However, fungal acne may look different for everyone since it depends on the cause. For example, thigh friction could encourage small bumps to form, but it could also make the skin dry and cracked. You should seek advice from your dermatologist to get the correct fungal acne treatment.
How to Get Rid of Fungal Acne? Effective Treatments and Tips
Your doctor should prescribe you topical or oral antifungal medications. These are the most effective treatments for protecting and replenishing your skin. If the fungal acne is more severe, you may require a long course of antibiotics to rebalance the yeast in your body.
To treat fungal acne at home, keep your skin clean and moisturized. Use face and body washes containing benzoyl peroxide, salicylic acid, or tea tree oil. These ingredients have anti-inflammatory and rapid microbicidal properties that could help to fight off yeast acne.
Exfoliating your skin with a gentle scrub or mitt can also remove dead skin cells that clog your pores. Do this once or twice a week to ensure your skin is soft and free from acne-causing bacteria like cutibacterium acnes.
You can also use anti-dandruff shampoos to treat fungal acne on your chest and back. This is because they contain zinc pyrithione and ketoconazole, both of which hold antifungal properties. Lather the shampoo in your hands and wipe that over the affected area. Leave it for 5 minutes and wash off with cold water.
How to Prevent Fungal Acne? 3 Ideas
You can prevent fungal acne by making simple changes to your routine. Even though antifungal treatments are most effective at protecting your skin, maintaining good hygiene is essential for preventing stubborn acne. Here are three ideas on where to start:
#1 Choose breathable fabrics
Start by wearing breathable clothes that don’t cause friction or excess sweating.
You should give your skin room to breathe so the yeast doesn’t multiply on moist and oily skin. Changing out of sweaty gym clothes as soon as possible can prevent a yeast infection.
#2 Use a proper cleanser
Use antifungal cleansers every day to warn off fungal and regular acne vulgaris.
Buy cleansers that contain ingredients such as benzoyl peroxide and salicylic acid to help clean your skin’s hair follicles and unclog pores. To maintain clean, healthy skin, try not to touch your face often since your hands can contaminate your follicles with germs.
#3 Eat nutritious foods
Lastly, follow a balanced diet for long-term fungal acne management and prevention.
Some antifungal foods include ginger, onion, garlic, apple cider vinegar, pumpkin seeds, and olive oil. These foods contain natural compounds that inhibit the growth of yeast and fungus. If you can, eat sugary foods in moderation, as sugar can cause acne by increasing inflammation.
FAQs
Yes, fungal acne can go away with topical treatments. You should speak to a doctor before using store-bought products that could make fungal acne worse. Antifungal creams are the best for relieving discomforts such as soreness and itchiness.
Using natural remedies alone may be difficult in the treatment of fungal acne, but you can use antifungal ingredients to manage your breakouts. Some include tea tree oil, apple cider vinegar, and thyme. However, more stubborn cases of fungal acne may require medication from a doctor.
Refined carbohydrates and sugary foods should be avoided, as they can cause blood sugar spikes and worsen the condition. A high lactose dairy product can also exacerbate fungal overgrowth in some individuals. Alcohol and fermented foods, such as bread and fermented products, can also contribute to fungi growth, so they should be avoided.
A Word From a Dermatologist
Acne is a frustrating and stubborn skin condition that strips your confidence. Those small, red bumps can also be agitating when you’re fighting the urge to scratch them. However, you shouldn’t have to deal with it longer than you should. By cleansing your face and wearing clean clothes, you can speed up the healing process.
There are some other tips to consider when treating your acne. One includes avoiding vaping as much as possible because the chemicals will damage your skin’s health. You should also use serums or cleansers containing hyaluronic acid, which is a natural substance that relieves dryness and soreness.
Drinking plenty of water can also prevent a microbial imbalance in your body. Women should drink 9 cups of water a day, and men need 12 cups. Hydrated skin also reduces inflammation and the stubborn yeast that causes fungal acne.
For more guidance on preventing and treating fungal acne, speak to your dermatologist about getting topical treatments.
Conclusion
So how is fungal acne treated?
Fungal acne is caused by malassezia yeasts infecting your skin’s hair follicles. A sweaty or moist environment can also cause fungal acne because the yeast has the chance to multiply in such conditions.
Therefore, cleaning your face regularly, changing out of sweaty clothes, and drying your skin are essential steps for preventing painful breakouts.
You can also consult with your doctor about oral antifungal medication or topical treatments to get rid of your acne.
















































 Select your language:
Select your language: 








